Treatment
In Europe survival from colorectal (bowel) cancer has increased over the past decade largely due to improved treatments and standards of care, however colorectal cancer is the most common type of cancer occurring, with deaths from it only exceeded by those from lung cancer. Treatment for colorectal cancer will depend on the stage to which the cancer has progressed at the time of diagnosis. Therefore each individual patient should have an individualised treatment pathway.
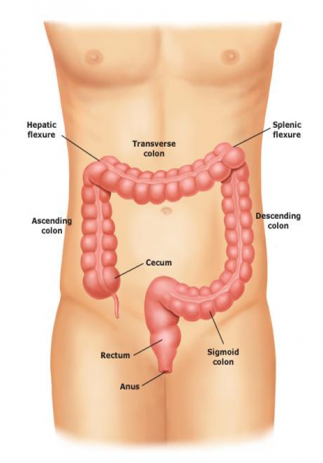
The Function of the Colon/Bowel
The colon is also known as the bowel or the large intestine.As the last part of the digestive system, the colonŌĆÖs main purpose is to extract water and salt from solid waste (faeces or stools) prior to the waste being eliminated from the body. The colon tends not to absorb food and nutrients, however it does absorb water, potassium and some fat soluble vitamins.
The colon consists of 4 sections: the ascending colon, the transverse colon, the descending colon and the sigmoid colon.
Surgery
Surgery is the primary treatment for removing a cancer from the colon.┬Ā┬Ā Unlike some other cancers where there are many treatment choices, surgery remains the most common treatment option for treating colorectal cancer.┬Ā In many cases this approach to remove colorectal cancer is highly successful and can be completely curative if the cancer is caught at an early enough stage.Many innovations have been made in the way colorectal cancer is treated with of the most effective and patient friendly innovations being the Enhanced Recovery Program.
The enhanced recovery program is about improving patient outcomes and speeding up a patient's recovery after surgery. It results in benefits to both patients and staff. The program focuses on making sure that patients are active participants in their own recovery process. It also aims to ensure that patients always receive evidence based care at the right time.
Outcomes of the enhanced recovery program are:
- Better outcomes and reduced length of stay
- Increased numbers of patients being treated (if there is demand) or reduced┬Ā┬Ā┬Ā┬Ā┬Ā level of resources necessary
- Better staffing environment
However, in some cases, the colon cannot be rejoined straight away, and a temporary colostomy is required.┬Ā┬Ā For most people, the stoma is temporary and can be reversed after a few months.┬Ā It is needed only until the colon or rectum heals from surgery.┬Ā After healing takes place, the surgeon reconnects the parts of the bowel and closes the stoma.
.png)
Radiotherapy
Radiotherapy is the treatment of cancer by deep X-rays. It is more commonly used to treat cancers of the rectum; this may be given before surgery to reduce the size of the tumour. This is called neo-adjuvant treatment. Radiotherapy can be used after the operation to make sure all the cancer cells are destroyed. This is called adjuvant treatment.Your radiotherapy treatment will usually be planned by an oncologist - a doctor specialising in treating cancer. In planning the radiotherapy, your doctor takes into account the size of the cancer, its sensitivity to radiation and the sensitivity of the surrounding tissues. He or she will also take into account your general health and fitness level. An example of Radiotherapy is SIRT.
.png)
Chemotherapy
In some cases surgery alone will not be enough to prevent the cancer from returning and in many cases further treatment may be required in the form of chemotherapy. Your chemotherapy regime will be prescribed by your oncologist. Chemotherapy is the use of anti-cancer (cytotoxic) drugs to destroy cancer cells. Chemotherapy drugs can stop cancer cells dividing and reproducing themselves; carried in the blood they can reach cancer cells anywhere in the body.Chemotherapy is normally given in a series of treatment sessions.. Each session is followed by a rest period. The session of chemotherapy and the rest period is known as a treatment cycle. A series of cycles makes up a course of treatment. The aim of having a rest period is to allow normal cells and tissue to recover from the treatment.┬Ā
.png)
Monoclonal Antibodies MAB (Biological Agents)
Monoclonal antibodies are a laboratory produced type of biological therapy and are a different type of treatment to chemotherapy. MAB can locate tumour cells and either destroy them or deliver tumour-killing substances to them without harming normal cells. They may also recruit the body's immune system to attack the target cells.┬Ā They do this by recognising certain proteins that are found on the surface of some types of cancer cells (known as receptors) and 'locking' themselves onto them..png)
About Biotechnology
Targeted/Personalised Treatments for Colorectal Cancer Patients
Biotechnology is providing doctors with more tools which are helping to move from the treatment of diseases to prevention and cure. A whole new range of tools are being developed to support the human body to utilise its own capacities to fight infectious or cancerous diseases as well as injuries. Greater understanding of disease and the causes of disease is helping to produce better therapies that can more effectively address medical needs. New insights into the biology of disease and more precise understanding of why some people react differently lie at the heart of biotechnology. The promise of more targeted/personalised treatments to individual groups of patients as well as providing treatments for diseases that so far have eluded treatment are providing us with new opportunities to meet challenging but common diseases like heart disease, cancer and AlzheimerŌĆÖs as well as rare diseases.
RAS is a new biomarker being used to select the best treatment for individual colorectal cancer (CRC) patients. The RAS gene in a CRC tumor may be 'wild-type' or 'mutant' and this RAS 'status' will help determine which treatment the patient is given. The test is very simple and uses tissue from the tumour which has already been removed. It should take about a week for you to receive the results.
Click for RAS Leaflet
┬Ā

Watch this video to learn more about RAS biomarker testing and its value for people newly diagnosed with metastatic colorectal cancer
Get Tested Campaign - 24th March 2015

| www.gettestedcampaign.com www.bowelcanceraustralia.org/get-tested Launched 24th March ┬Ā |
 Jola Gore-Booth was a speaker at the launch of the Get Tested Campaign in Brussels from the 24th of March. RAS Biomarker Testing is vitaly important to patients yet a recent survey showed that only 45% of patients in Europe with advanced Colorectal Cancer believe that a test can indicate if a particular cancer drug could work. ┬Ā |
| Press Release |
| Infographic 1 Get Tested Press Release Infographic 2 Get Tested BioMarker Infographic┬Ā |
| White Paper Robyn - Patient Story┬Ā |




-(2).png)

